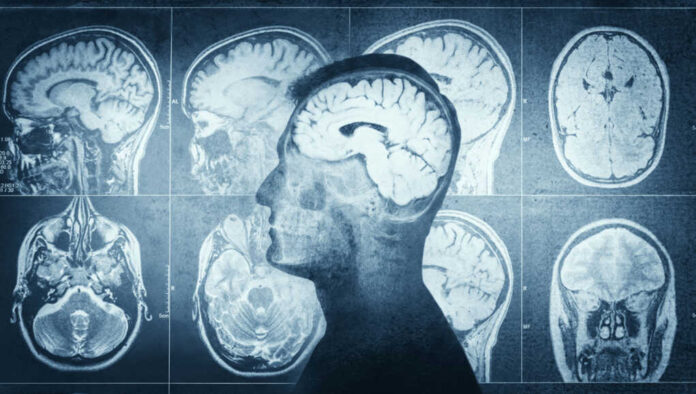
Neurons possess a secret cellular arsenal that shreds toxic tau proteins, potentially unlocking affordable therapies to halt Alzheimer’s before it ravages the brain.
Story Highlights
- UCLA and UCSF researchers discovered the CRL5SOCS4 complex, a natural cleanup system targeting harmful tau fragments for degradation.
- CRISPR screening on human stem cell neurons revealed why some brain cells resist Alzheimer’s tau buildup.
- Mitochondrial stress links to specific tau biomarkers like NTA-tau, validated in actual Alzheimer’s tissue.
- Shift from amyloid plaques to tau resilience promises cheaper drugs over costly antibodies.
Discovery of Neuron Resilience Mechanism
Dr. Avi Samelson led researchers at UC San Francisco, now at UCLA Health, to identify the CRL5SOCS4 complex. This ubiquitin ligase marks toxic tau proteins for proteasome degradation. Tau tangles destroy neurons in Alzheimer’s and frontotemporal dementia. Some neurons survive intense pathology. CRISPR-based genetic screening on human stem cell-derived neurons pinpointed this defense. The team used disease-mutant models for direct relevance to human disease.
Linking Mitochondrial Stress to Tau Pathology
Mitochondrial dysfunction triggers harmful tau fragments, including NTA-tau biomarker. CRL5SOCS4 specifically degrades these fragments. UFMylation emerges as another novel pathway regulating tau. Validation occurred in human Alzheimer’s brain tissue, confirming real-world applicability. Prior research puzzled over neuron-type vulnerability variations. This work explains resilience through targeted cleanup, not universal weakness.
Historical Context in Alzheimer’s Research
Alzheimer’s targets amyloid-beta plaques and tau tangles. Tau aggregates damage neurons unevenly across brain regions like the hippocampus. Genetic screens previously lacked human neuron specificity. Advances in CRISPR and stem cells enabled genome-wide analysis. Precedents include SST1/SST4 receptors boosting amyloid clearance and LilrB2 synapse pruning. FDA-approved lecanemab mobilizes microglia against amyloid, but tau persists as the dominant pathology.
Key Stakeholders Driving Progress
Dr. Avi Samelson authored the study, identifying CRL5SOCS4 links. UCLA Health and UCSF supplied stem cell neurons and CRISPR technology. Cell journal published the peer-reviewed paper on March 3, 2026. Per Nilsson at Karolinska advanced SST1/SST4 for amyloid. Carla Shatz at Stanford explores LilrB2 pruning. Teams target treatment gaps for 50 million global dementia cases. Academic collaborations fuel discoveries without noted conflicts.
Recent Developments and Statements
The Cell publication marks the breakthrough on March 3, 2026. Samelson stated, “Boosting this natural cleanup pathway could form the basis of new therapies.” No post-publication updates emerged by March 4. Related February 2026 findings cover SST receptors, IDOL enzyme deletion reducing plaques, and exercise-induced brain repair. Preclinical status demands animal and human trials. CRL5SOCS4 pathways suit drug targeting.
Potential Impacts and Expert Views
Short-term, NTA-tau validates diagnostics. Long-term, enhancing CRL5SOCS4 slows progression, complementing amyloid drugs. Economic shifts favor cheap pills over $26,000 annual antibodies, aligning with conservative values of practical, cost-effective solutions grounded in biology. Nilsson praises receptor drugs as safer. Shatz flips microglia focus to neuron pruning. Consensus urges multi-pathway therapies amid translation challenges.
Sources:
Scientists just found the brain’s hidden defense against Alzheimer’s
IDOL enzyme deletion in neurons reduced plaques
Exercise-induced liver protein repairs brain
Expanding the Alzheimer’s treatment landscape: A 2026 forecast
Pharmacologic reversal in tau mice via P7C3-A20