Your body possesses a hidden biological brake that can shut down runaway inflammation before it destroys your joints, damages your heart, or fuels chronic disease—and scientists just figured out how to activate it on command.
Story Snapshot
- University College London researchers identified fat-derived molecules called epoxy-oxylipins that naturally stop inflammation by blocking harmful immune cells
- A repurposed drug accelerated pain resolution in human volunteers by boosting these molecules without suppressing the entire immune system
- The discovery targets intermediate monocytes, immune cells that drive arthritis, heart disease, and other chronic inflammatory conditions
- This represents the first human proof that the body’s resolution phase can be therapeutically controlled, unlike broad immunosuppressants
The Body’s Biological Dimmer Switch
University College London scientists unveiled a mechanism that reads like your immune system’s version of a thermostat. Published in Nature Communications this February, the research demonstrates how molecules called epoxy-oxylipins—fat metabolites your body naturally produces—act as a regulatory brake on inflammation. When researchers administered a drug blocking soluble epoxide hydrolase, the enzyme that degrades these molecules, volunteers experienced faster pain relief after controlled inflammation. The kicker: visible swelling remained unchanged, but the internal cellular chaos quieted down. This distinction matters because it targets the problem at its source rather than masking symptoms.
https://youtu.be/iK0tdwMZul8?si=Bmn7yKkOtgcEi9iY
Intermediate Monocytes: The Inflammation Agitators
The study zeroed in on intermediate monocytes, a subset of white blood cells that transition between inflammatory and healing states. These cells accumulate in chronic conditions like rheumatoid arthritis and cardiovascular disease, perpetuating tissue damage long after the initial threat disappears. Dr. Olivia Bracken and Professor Derek Gilroy demonstrated that elevating epoxy-oxylipins prevented these monocytes from multiplying in both blood and inflamed tissue. The specific molecule 12,13-EpOME achieved this by inhibiting the p38 MAPK signaling pathway, a critical switch that normally tells immune cells to expand and attack. This isn’t speculation based on mouse models—UCL conducted these experiments on healthy human volunteers using controlled bacterial challenges.
Repurposing Existing Drugs for Safer Treatment
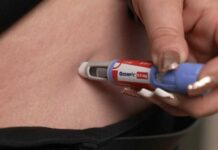
The drug tested, GSK2256294, already exists with established safety profiles, eliminating years of regulatory hurdles for potential clinical applications. Volunteers received the compound either two hours before inflammation induction or after onset, mimicking both preventive and therapeutic scenarios. Results showed the drug worked in both contexts, accelerating the resolution phase without the immune suppression risks associated with steroids or biologics. This approach preserves your body’s ability to fight infections while dialing down the destructive overshoot that characterizes chronic inflammation. For millions suffering from conditions where current treatments essentially carpet-bomb the immune system, this precision represents a paradigm shift toward restoring balance rather than imposing blanket suppression.
Beyond Animal Models to Human Validation
Previous research hinted that epoxy-oxylipins might regulate inflammation based on animal studies, but translating rodent biology to human physiology notoriously fails. The UCL team bridged that gap by injecting UV-killed E. coli bacteria under volunteers’ skin, creating measurable, reproducible inflammation without actual infection risk. They tracked pain levels, immune cell counts, and molecular markers throughout the resolution process. The human data confirmed what animal models suggested but couldn’t guarantee: blocking soluble epoxide hydrolase genuinely amplifies the body’s natural shutdown mechanism. This validation matters because pharmaceutical companies won’t invest in clinical trials without human proof-of-concept, and patients won’t benefit from discoveries that never escape the laboratory.
The Chronic Inflammation Epidemic
Chronic inflammation underpins conditions afflicting hundreds of millions globally—arthritis that gnarls joints, atherosclerosis that chokes arteries, diabetes that ravages organs. Current treatments often involve corticosteroids that weaken bones and raise infection risk, or biologics costing tens of thousands annually while suppressing immunity broadly. The epoxy-oxylipin pathway offers an alternative: enhancing resolution rather than blocking initiation. Professor Gilroy emphasized designing safer treatments for diseases currently bereft of targeted therapies. The economic implications extend beyond patient health; chronic inflammatory diseases drain healthcare systems through hospitalizations, disability, and lost productivity. Repurposing existing drugs could accelerate availability while reducing development costs, a rare convergence of medical and fiscal responsibility.
Scientists discover the body’s hidden “off switch” for inflammation via @ScienceDaily: https://t.co/EmyQBgMUWc #Inflammation #InflammationOffSwitch #AMMG #AgeManagementMedicine #CMEEducation #ContinuingMedicalEducation #CMEConferences #AMMGMembership #Certification pic.twitter.com/FQ5tGTgIh3
— AMMG (@AgeMgmtMedGroup) February 19, 2026
The research distinguishes itself from unrelated “kill switch” discoveries making headlines simultaneously. The Doherty Institute identified a T-cell mechanism involving P2RX7 receptors and NAD molecules, while UT Southwestern found an obesity-inflammation switch—both valuable but addressing different cellular processes. The UCL work specifically targets the resolution phase through fat-derived molecules, a fundamentally distinct biological strategy. Clarity matters here because sensationalized “breakthrough” coverage often conflates separate findings, creating confusion about what actually works and when clinical applications might arrive. The UCL study’s human validation and drug repurposing potential position it closer to bedside implementation than most laboratory discoveries ever reach.
Sources:
Scientists discover the body’s hidden ‘off switch’ for inflammation – ScienceDaily
Scientists discover natural brake that could stop harmful inflammation – UCL News
Scientists Discover the Body’s Natural Off Switch for Inflammation – SciTechDaily
How to Stop Inflammation in the Body – Prevention
Researchers discover how to turn off chronic inflammation – KFF Health News