According to new research, antibodies obtained from common food allergies could also increase your risk of heart disease. This article examines this claim and the effect of food allergies on your heart health.
What Do The Researchers Say?
A team from the University of Virginia Health (UVA) System said these IgE antibodies don’t have to be present in quantities high enough to produce an actual food allergy required to have this unhealthy effect on the heart.
Dr. Jeffrey Wilson said the team examined the presence of IgE antibodies in food detected in blood samples. He also said the team didn’t think most of the study’s subjects had overt food allergy, so they only analyzed the silent immune response to food.
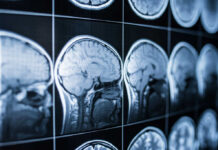
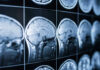
Dr. Wilson said these responses might not be strong enough to cause acute allergic reactions to food. However, he said they can cause inflammation and eventually result in heart disease.
This can be an issue for most individuals as about 15% of adults produce IgE in response to foods like cow’s milk and peanuts. That said, not everyone who produces the antibodies will have a symptomatic food allergy.
How Was The Study Conducted?
During their research, Wilson’s team collected data on nearly 5,400 individuals involved in either a study of heart disease centered in Wake Forest, N.C., or a national U.S. health data bank. In total, 285 of the participants from both data sets died due to heart disease.
The researchers said the more extensive national study recorded IgE antibodies in at least one food were linked to a higher risk of cardiovascular death. They also said that the presence of milk allergies seemed to have the most vital connection to cardiac death, alongside antibodies linked to peanut and shrimp allergies.
What Does This Mean for Heart Health?
Dr. Wilson’s team currently only has theories on the link between allergies and heart health. They said allergic antibodies could trigger specific cells in the skin and gut to cause allergic reactions. Unknown genetic and environmental factors might also explain the connection.
The researchers said more studies are required, but these new insights into allergens and the heart could eventually help patients. Wilson said their work suggests that future blood tests could provide personalized information about a heart-healthy diet.
Conclusion
Recent studies suggest that specific antibodies caused by food allergies can increase your risk of heart disease. While further studies are needed, this research could help physicians improve their patients’ heart health.